For Doctors
You are probably on this website because a patient showed it to you. Here is what you need to know:
Symptoms
The symptoms of Short QT Syndrome can include:
- bradycardia
- heart palpitations, extrasystoles
- atrial fibrillation
- dizziness, fainting, syncope
- ventricular tachycardia
- cardiac arrest, sudden cardiac death, ventricular fibrillation
These symptoms can occur at a very young age.
Diagnosis
On an ECG, Short QT Syndrome may look like this:
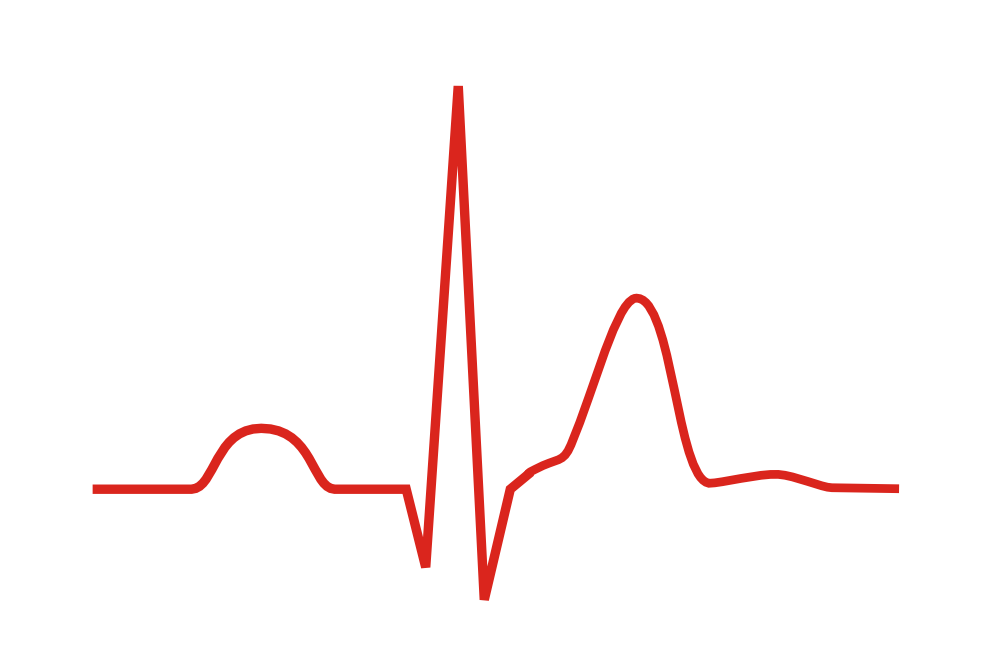
The QT interval is shortened. T waves as tall as the R wave can also occur:

The exact cut-off values for a short QT interval are a topic of discussion.
According to ESC Guidelines 2022, Short QT Syndrome is diagnosed in the presence of a QTc equal or lower than 360 msec and one or more of the following:
- a pathogenic mutation
- a family history of SQTS
- survival from a VT/VF episode in the absence of heart disease
SQTS should always be considered in the presence of QTc equal or lower than 320 msec (2015: 340 msec).
SQTS should be considered in the presence of QTc between 320 ms and 360 msec and arrhythmic syncope.
SQTS may be considered in the presence of QTc between 320 ms and 360 msec and a family history of sudden death at age lower than 40 years.
There are usually no structural heart defects, the ultrasound is inconspicuous.
Statistical analysis using large-scale studies
A few studies tried to determine the distribution of QTc values in the general population. One of these studies is presented here: Vandenberk et al., 2016. Please keep in mind that there are different results from other researchers.
According to that study, the distribution of QTc values in the general population looks like this (Fridericia's correction formula):

You can see a lot on this graphic (it shows values of women and men combined). The median is at 414 msec (black line). Two standard deviations to the left, we find 364 msec (another black line). That seems to correspond to the recommendations from the ESC which demand a value lower than 360 msec. Only about 1.5 % of the population have QTc intervals equal or lower than 360 msec. Virtually no one (approximately 0.008 %) has a QTc interval equal or lower than 320 msec. You can see now why the 320 msec cutoff is very strict. The older cutoff value from 2015 (340 msec) was a bit more generous, with 0.15 % of the population.
On the other hand, the cutoff value of 320 msec yields a bit more than 600,000 people worldwide (assuming the Vandenberk study is correct). The definition of a rare disease is often given as 1 in 10,000 people, which would be around 780,000 people on earth. These two values correspond pretty well.
How many patients are there?
Statistically, there should still be many patients with a short QT interval, given the world's considerable population (as shown in the paragraph above). Reported are less than 300. It is yet unclear why that is.
Comparison to Long QT Syndrome
Let's have a short look at the Long QT Syndrome. Its absolute cutoff value of 480 msec is 20 msec above the relative cutoff value of 460 msec (which again corresponds to the second standard deviation of 464 msec). In Short QT Syndrome, a distance of 40 msec has been chosen.
Gollob Score
In 2011, Gollob et al. proposed a scoring system, similar to the widely used Long QT Score (originally from Schwartz et al.). It is unclear whether this score is useful in diagnosis, and it has not been adopted by consensus guidelines. For that reason, use of this score is discouraged. Stick to the consensus guidelines.
Finding the right correction formula for QTc
Use of a correction formula in diagnosis of SQTS is disputed. The relationship between the length of the QT interval and heart rate is sometimes altered in SQTS patients. Therefore, it is recommended to obtain an ECG close to 60 bpm, in order to keep the influence of the correction formula low. Some doctors suggest not to use a correction formula at all, but this has not been adopted by international consensus guidelines.
Please be aware that Bazett's formula sometimes over- and undercorrects. Use another formula. You can use our QTc calculator for calculation.
Genetics and cellular mechanisms
Several gene mutations have been associated with short QT intervals. It has been tried to link them to individual phenotypes, but it is unclear if these links are correct (and for that reason, they are not presented here).
The following genes have been implicated so far: KCNH2, KCNQ1, KCNJ2, CACNA1C, CACNA2D1 and SLC4A3. Some researchers assign them numbers from 1 to 6. Some newer research confirmed only a subset of them. In some cases of a CACNA1C mutation, the short QT interval is accompanied by a Brugada phenotype, but it is unclear if that is definitive for all cases.
Risk stratification
Risk stratification in Short QT Syndrome is extraordinarily difficult because there are so few cases.
There is a study by Mazzanti et al., 2014, that has determined the risk of sudden cardiac death to be higher than 40 % by the age of 40, but this study is heavily disputed (selection bias).
Treatment
ICD implantation is recommended by consensus guidelines in patients who are survivors of an aborted cardiac arrest and/or have documented spontaneous sustained ventricular tachycardia. Due to tall T waves, a special programming of the ICD is often required (“T Wave Oversensing“).
In other patients, Quinidine may be used. It is the only medication that has been proven effective so far. Unfortunately, although it is an old substance, nowadays it is only available in a few countries and frequently has to be imported.
We can recommend the English Wikipedia article about SQTS.
Also, follow us on Twitter! http://twitter.com/shortqtsyndrome
